Hip Arthritis and Total Hip Replacement
LOADING
What is hip arthritis?
Any condition that causes the slippery cartilage surfaces to break down and no longer glide smoothly will result in a painful, stiff hip joint – just like a rusty hinge – if it doesn’t glide smoothly, it will catch or have a grating sensation from time to time, and even occasionally make an unusual click. In the human body, this leads to symptoms of pain and stiffness in the groin, lower back or even the buttock. There are a large variety of causes for hip cartilage to break down and the joint to become arthritic, but the end result is essentially the same.
As a result of the cartilage breaking down, the space between the bones, normally made up by the cartilage and synovial fluid, breaks down and becomes narrow. The body attempts to “heal” itself and so it will often form large spurs of bone, the capsule of the joint will become thickened with inflammation, and small pockets (cysts) may form in the surrounding bone. These are the hallmarks of arthritis.
Diagnosis
The diagnosis is usually made by Mr Robin taking a history and performing a physical examination. More often than not, this information provides the majority of the clues to the diagnosis. Almost always, a simple set of X-rays of the hip and pelvis will then be used to confirm the diagnosis, and can also be used to better examine the severity of disease, as well as plan any surgery if required.
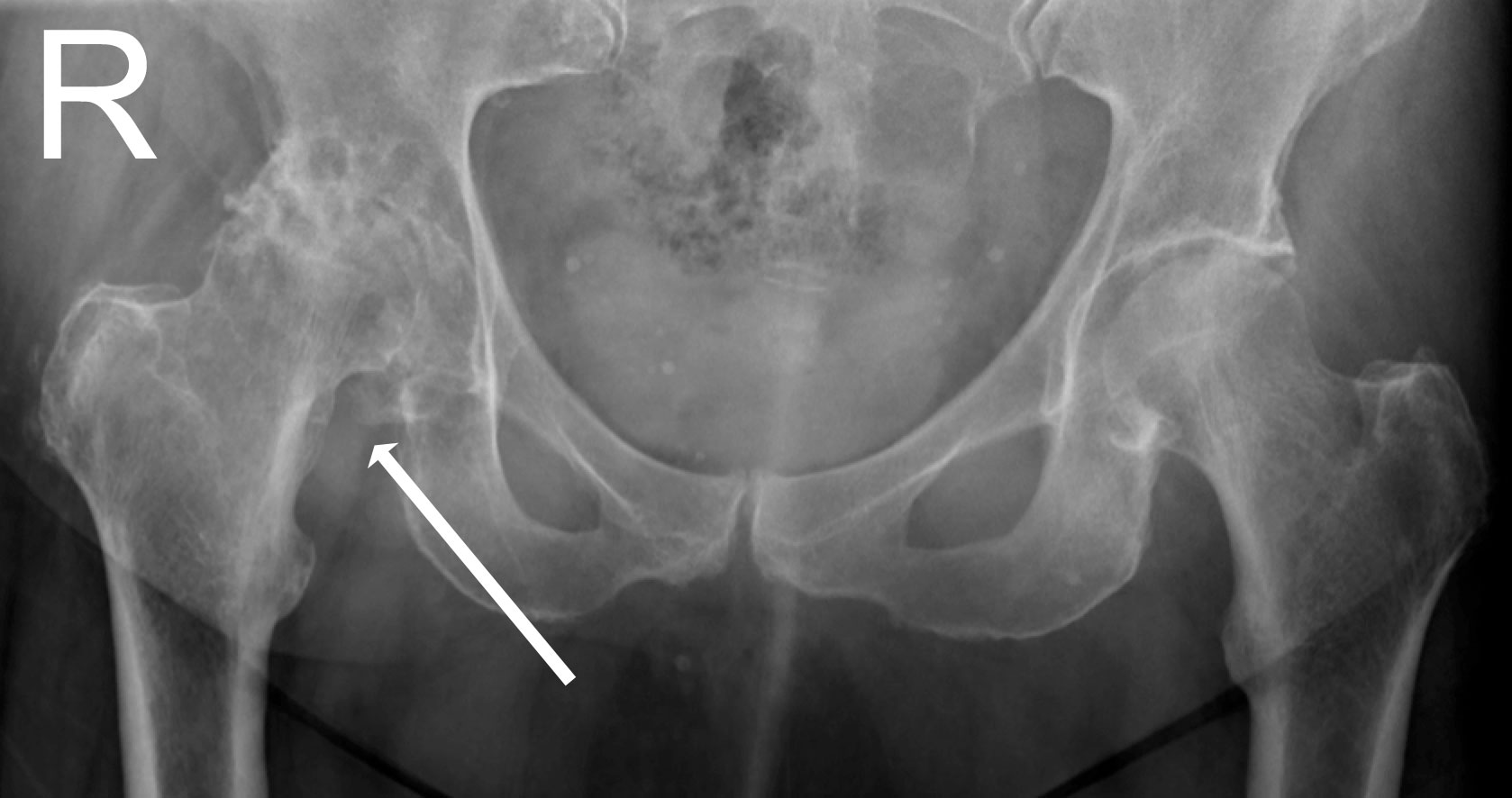
X-ray of Arthritic Hip (Right)
Natural History
If left untreated, unfortunately, osteoarthritis of the hip does not get better by itself and does not “heal” on its own. There will be periods where the symptoms may get better for a while (e.g. in warmer weather or with less activity), but invariably it will deteriorate again and gradually the pain will increase in severity or frequency, as will limping and stiffness.
Non Operative Treatment
In most cases, non-operative treatment should be trialled before undergoing hip surgery. This initially involves modifying ones lifestyle to accommodate their abilities – e.g. cutting back on sports, walking shorter distances if possible, carrying lighter weights. After this, oral medications such as paracetamol (Panadol/Panadol Osteo), anti-inflammatories (ibuprofen, indomethacin, meloxicam, diclofenac), and opiate-based medications (codeine, oxycodone) can be used to help reduce any pain. Some patients may be willing to use a walking stick, although this may be considered less socially acceptable in the 21st century, it is still a reliable and effective means of managing an arthritic joint in the leg. Some patients may find hydrotherapy and physiotherapy techniques useful to manage pain, reduce stiffness, maintain muscle bulk and whatever flexibility their joints may have, as well as keeping their weight under control.
Operative Treatment
When the symptoms from the arthritic hip joint are no longer tolerable or manageable by non-operative methods, then patients will often consider surgical treatment. For hip arthritis, the most reliable and enduring procedure in the overwhelming majority of cases will be a form of hip replacement (or hip resurfacing – in younger male patients). The nature and method of hip replacement/resurfacing may vary considerably between various surgeons or even within a single surgeon’s practise (e.g. the same surgeon may use hip replacement “Type A” for younger patients and “Type B” for older patients, or alternatively these may vary depending on the patient’s anatomy or the underlying cause of the arthritis, for instance). Discussion of the various types and techniques of total hip replacement is beyond the spectrum of this website – entire volumes of textbooks have been dedicated to this procedure and even still, dozens of scientific studies on the various features of hip replacements are being published every month in numerous orthopaedic journals around the globe. Clearly there is no single “best” type of hip replacement or “best” way to do it. It’s often a case of “horses for courses”.
The information above is general. All surgical procedures involve some risk. If you would like advice on your specific condition, please contact the office of Mr Daniel Robin, Melbourne Orthopaedic Surgeon.

