Fractures
LOADING
What is a fracture?
A fracture is ANY break or loss of continuity in the structure of a bone, whether it is a tiny crack all the way up to a bone that has split into multiple fragments.
Fractured bones may be undisplaced (a tiny crack in the bone without any significant separation of the fragments) or displaced (where there is a detectable deformity in the bone).
Different types of fractures
In normal bones, fractures usually occur when sudden amount of high force is applied to the bone. A “pathological fracture” is a fracture that occurs in a bone with abnormally reduced strength that experiences otherwise normal forces. There are a number of different causes of bone weakness, including osteoporosis, genetic abnormalities in bone formation and maintenance, developmental abnormalities of bone, non-cancerous and cancerous tumours, and infections.
Stress fractures occur in normal bones, but these bones are exposed to excessive/repeated loading and unloading, above what would be considered normal everyday activities. They are frequently seen in the lower limbs of athletes who run or jump, or soldiers who march long distances with heavy packs (e.g. stress fractures in the metatarsals of the feet or in the lower end of the tibia).
How can it be treated?
Most fractures tend to mend if the ends/surfaces of the broken bone are very nearby and the fine tissue lining the bone (periosteum) is relatively intact. When the bone breaks, the bone marrow bleeds and forms a clot (over a few hours) which is gradually converted by cells in the periosteum into fibrous scar tissue initially (over a few weeks) and this is later converted into calcified tissue (a few weeks or months later) – i.e. a basic form of bone again. With time this basic bone is then matured into more normal bone over a few more months. This is a biological process which is unable to be accelerated, generally, however, in some instances the healing process can be slowed down beyond what is normally seen. In particular, smoking tobacco in any form will essentially poison the cells responsible for converting the blood clot into calcified tissue and will reduce the rate of healing of a fracture. In many cases, smoking may stop healing altogether, and when this occurs it is called a “non-union”. Patients on bisphosphonate medication e.g. aledronate (Fosomax), pamidronate (Aredia) and residronate (Actonel) for Osteoporosis will frequently have a delay in healing or even non-union. Diabetics are also known to have a reduced rate of healing fractures. Some bones in particular are known to have a poor blood supply and may be more prone to non-union such as the neck of the femur, the scaphoid bone in the wrist, the neck of the talus in the ankle and the shaft of the tibia. If the fragments of bone that has a normal healing potential are separated by a long distance (which usually means significant damage to the healing periosteum), they may also fail to heal.
For healing to occur, not only must the ends of the bone be nearby, but the fragments usually need to be immobilised for sufficient time for the healing process to get under way. This also depends on the location of the fracture and the age of the patient. In general, children tend to heal more rapidly than adults and upper limb injuries tend to heal more quickly than lower limb injuries. Again, this depends somewhat on which bone (and sometimes which part of the bone) is fractured.
The methods of treatment of fractures can take many forms, but can broadly be grouped into “closed” and “open” methods. Closed methods utilise techniques where the broken bone itself is not directly manipulated, but is done so indirectly by applying gentle but firm pressure on the bone with the skin and muscles left intact – i.e. no incisions are made and the bone is not “seen” by the surgeon. These include the use of external immobilisation of the broken bone by use of a splint or brace, a circumferential plaster cast or an external fixateur. Open methods involve the surgeon making an incision in the skin and splitting muscles to allow direct manipulation of the broken bone ends so that they are accurately placed as close as possible to their original position. Open techniques include internal fixation with plates and screws on the external surface of a bone, and with intramedullary rods which are implanted within the bone marrow of the bone.
Closed Treatment of Fractures
The simplest method is to use an external splint or brace which may be worn under or over clothing to hold the limb/broken bone still. This has the advantage of being removable, not overly constrictive, and its position may be adjusted if there is swelling. As there is no incision made in the skin, there is no risk of infection, bleeding or nerve and blood vessel injury. However, this is also a disadvantage as the fractured bone may be permitted excessive mobility and then may fail to heal/unite.
A cylindrical/circumferential cast is more conforming and restrictive than a splint. This is made out of Plaster of Paris or synthetic material such as fibreglass or casting tape. This cast encloses a portion of the broken limb and has the advantage of being highly conforming and thus very good at immobilising the fracture, as long as there is minimal swelling. It also doesn’t run the risks of surgery such as infection, bleeding or nerve and blood vessel injury.
Closed management of fractures does not always allow precise placement of bone fragments if they have been significantly displaced, unless an anaesthetic is administered to permit the surgeon to manipulate of the fracture fragments (without making any skin incisions). This is called a “closed reduction” or a GAMP (General Anaesthetic, Manipulation and Plaster).
If the fragments of bone are too unstable or to large to be managed in an external splint or plaster (e.g. a fractured femur), one option may be to use multiple heavy pins which pass from outside the skin into the broken bones, and then to connect these pins to larger rods to form an external frame, linked to the bone. This is called “external fixation”, and has the advantage of having a solid, direct grip on the bone fragments but without disturbing the soft tissues around the bone and allowing the fracture to be reasonably well immobilised. The disadvantages of this technique include infection of the muscle/bone by the patients skin germs tracking down the external surface of the pins, the pins may loosen from the bone, the fixation may not be strong enough to permit immediate or early weight bearing or range of movement, and there is a small chance of nerve or blood vessel injury. The pins also need to be removed eventually, sometimes requiring a further anaesthetic to do this.
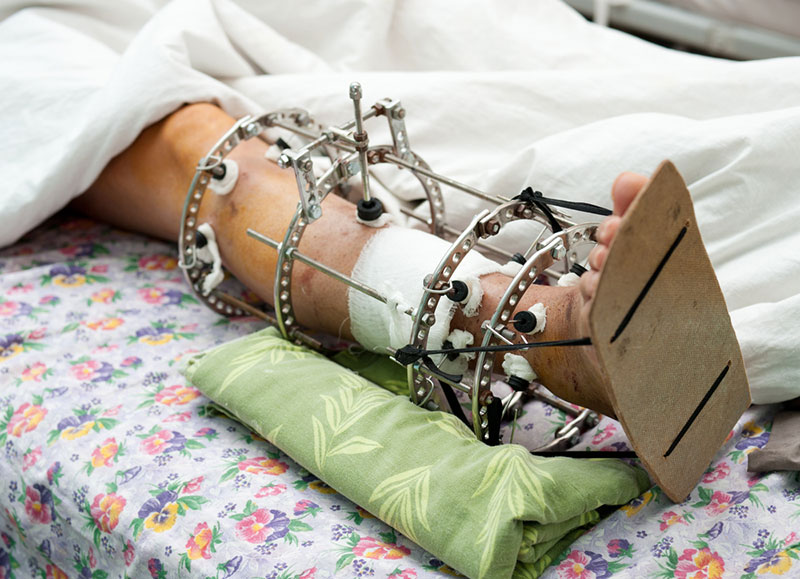
External fixation
Open Treatment of Fractures
If the fracture fragments are more significantly displaced, or involve the surface of an important joint then open methods of fracture management may be required. The surgeon will perform an “open reduction”, where an incision is made in the skin, the muscles and other vital structures like nerves and arteries are moved to allow visualisation of the broken ends of the bone and bring them closer together with less deformity. With fractures that are significantly displaced and risk progression to a non-union, this technique is used to bring the bone ends close enough enable the fragments to heal, and has the advantages of permitting healing with much less deformity, earlier movement of the joints on either side of the broken bone (as the fracture has been stabilised internally by a rod or a plate and screws), or earlier bearing of weight.
Open Reduction and Internal Fixation (ORIF) of fractures will not necessarily increase the speed at which the fracture heals, but makes healing more certain and should reduce the amount of deformity/disability encountered if the same injury were to be treated by closed means.
Fractures that involve the cartilage surfaces of important joints such as the wrist, elbow, shoulder, hip, knee and ankle usually have a higher probability of developing post traumatic arthritis (pain and stiffness) if the fragments of bone have greater than 2mm of separation at the surface of the joint.
ORIF has the disadvantages of infection, bleeding, nerve and vessel injury and occasionally may require secondary surgery to remove implants once the fracture has healed if they cause irritation of nearby structures or prominence under the skin. Fortunately, these problems are not common.
The information above is general. All surgical procedures involve some risk. If you would like advice on your specific condition, please contact the office of Mr Daniel Robin, Melbourne Orthopaedic Surgeon.

